Select Health offers a variety of online tools that make it easier for you and your team to get the information you need, right when you need it. Whether you’re checking a patient’s benefits, looking up claim details, or submitting a preauthorization, these tools are designed to save you time and simplify your day-to-day work. With quick access, intuitive features, and secure systems, managing patient information has never been more convenient.
- Provider Benefit Tool (PBT): Verify benefits, eligibility, and claims status
- Preauth & Care Plan Tool: Submit preauthorization requests, monitor request status, and view decisions
- How to Register
Provider Benefit Tool (PBT)
Search options within the tool help you locate patients, claims, or remittance advice. Other features allow you to:
- Search for benefits and eligibility information by Select Health member ID number, Medicaid ID number, name and date of birth, or Social Security number.
- View a patient’s claims history and status or processing information by individual claim or member.
- Securely request a reprint of a Remittance Advice/ Explanation of Payment.
- Attach supporting documents to a specific medical or dental claim (when required) to facilitate reprocessing.
- View medical and dental member payment summaries, which provide more benefit details.
- Quickly locate deductible and out-of-pocket accumulators.
- Access outpatient physical, speech, and occupational therapy accumulators.
- View coordination of benefits information to help determine the order of benefits for a member (if applicable).
- View medical and dental coverage history.
Visit selecthealth.org/providers/claims/pbt to learn more.
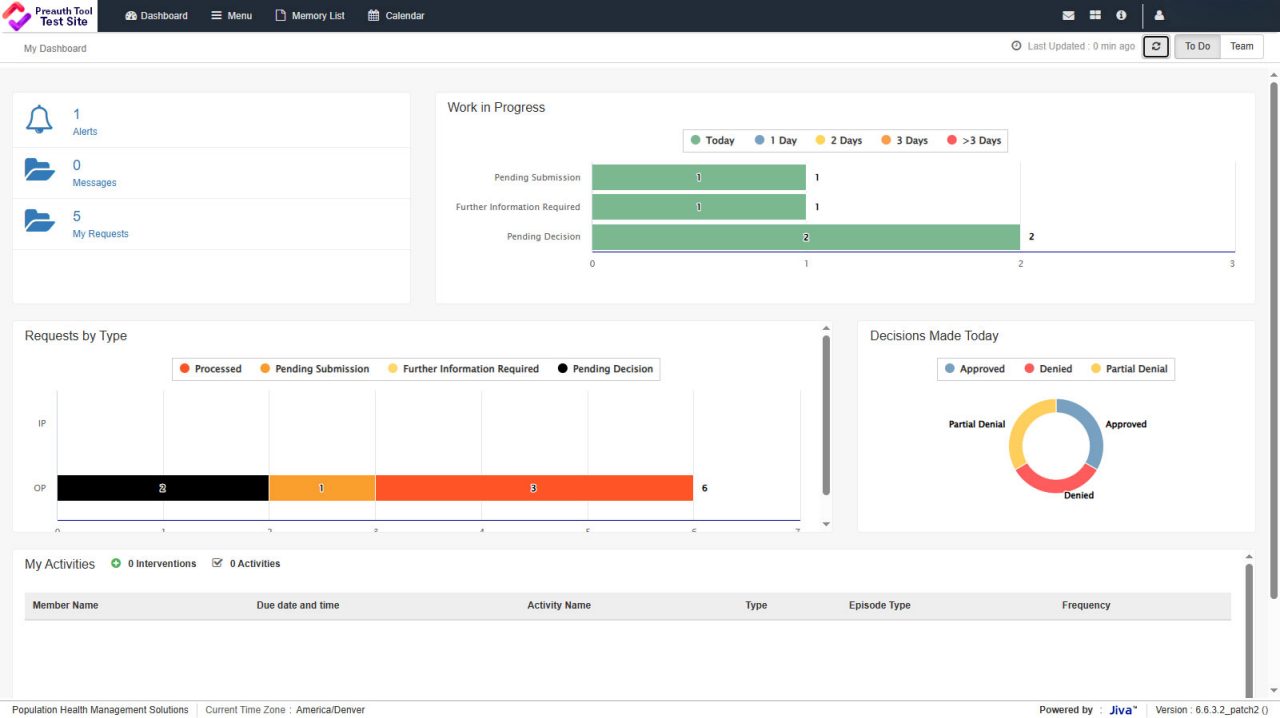
Preauth & Care Plan Tool
Using the Preauth & Care Plan Tool means:
- Fewer overall required steps to preauthorization for your patients
- No more duplicative efforts and potential errors when staff enter information from a paper form
- Reduced response time, follow-up calls, and decision delays due to missing information
- No risk of faxed member information being lost or sent to the wrong fax number
- Automatic review and preauthorization decisions for many procedures
Visit selecthealth.org/providers/preauthorization/preauth-care-tool to learn more.
Register to Access Select Health's Online Tools
Ready to start using our online tools? You can register for access to both the Provider Benefit Tool and the Preauth & Care Plan Tool by following the steps below.
Get a Secure Access Login
Email all completed documentation to providerwebservices@selecthealth.org.
*Note: If you are adding a user to an existing account, you only need to submit the login application.