Preauthorization
By
May 05, 2026
Speed up the preauthorization process in your office by having your staff sign up for the Preauth & Care Plan Tool to submit and monitor requests online. Compared to faxed and emailed requests, this tool can make the process easier than ever, with many benefits like:
- Reduced response time
- 24/7 preauthorization status information
- No risk of information being lost, sent to the wrong number, or other errors
- Reduced follow-up calls and decision delays due to missing information
- Automatic review and preauthorization decisions for many procedures (including CPAP/BIPAP, eye procedures, hysterectomy, spinal pain interventions, tonsillectomy/adenoidectomy, total joint [hip and knee], and varicose vein procedures.) Learn more.
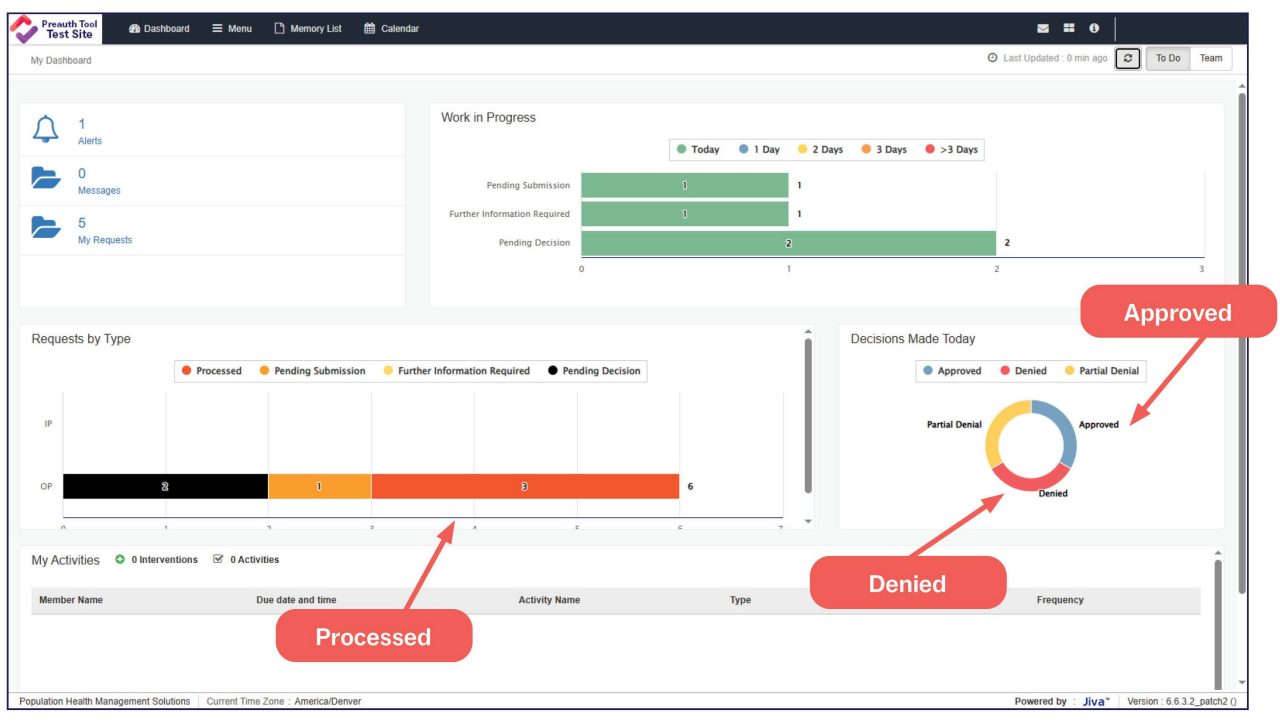
Updates for Current Users
Some users have encountered the following common issues when logging in or creating authorization requests. Please read the information below to learn what steps you should take to resolve these problems if needed.
- Login Errors: If a registered user receives a TaxID XML error when trying to login, please call the help desk at 801-442-7979, option 2 to submit a ticket. Please include the error message in your ticket.
- Limit Requests to 10 Diagnosis Codes: When submitting a preauthorization request in the Preauth & Care Plan Tool, do not include more than 10 diagnosis codes at a time. This may cause issues with the system.
- DME Ordering Providers: Please add the ordering provider (requesting provider) to all requests so that decision letters can be sent to the ordering provider.
Nevada Medicare Providers
The Preauth & Care Plan Tool is not available for Medicare providers treating Medicare members who live in Nevada. Contact Nevada Provider Relations with any questions.
Training & Other Resources
Check out the Preauth & Care Plan Tool page for more helpful resources, including:
Other News
Use Our Online Tools for Faster Claims & Preauth
Learn more about our online tools that make it easier for you and your team to get the information you need, right when you need it.
Read more

Solutions to Common Preauth Tool Issues
Many common issues can be solved with a few quick actions. Please read this information to learn what steps you should take to resolve these problems.
Read more
Get Started with the Preauth & Care Plan Tool
Still faxing your preauthorization requests? Let the staff at your practice know that they can sign up for the Preauth & Care Plan Tool to submit and monitor requests online, making the process easier than ever.
Read more
Update: Adding Contact Info in the Preauth & Care Plan Tool
You will now see a new section, Contact Details, when creating an authorization in the Preauth & Care Plan Tool.
Read more